For those with addiction, going into and coming out of prison can be a minefield. : NPR

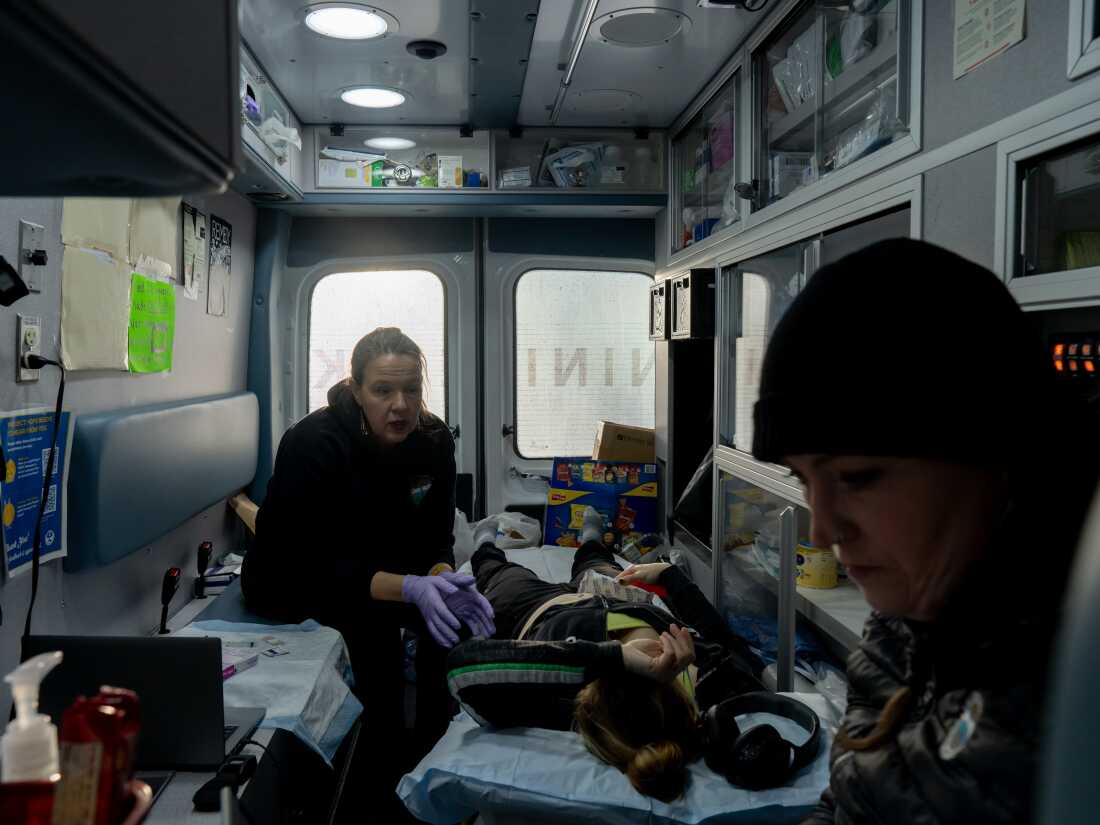
Dr. Sarah Spencer and case manager Annette Hubbard see a patient in the mobile clinic outside a shelter in Kenai, Alaska, November 20, 2025.
Ash Adams for NPR
hide caption
toggle caption
Ash Adams for NPR
At Ninilchik Community Clinic this summer, on Alaska’s rural Kenai Peninsula, Dr. Sarah Spencer stood next to a patient lying on an examining table and doused her stomach with alcohol. The patient was there for a monthly buprenorphine injection to treat her opioid use disorder — an injection she thought might be her last for some time since a warrant had been issued for her arrest. The Alaska Department of Corrections does not provide full access to this life-saving medication.
“I’ll give you a little pinch,” Spencer said, sliding the needle into a fold of skin on the patient’s stomach for the subcutaneous injection.
Alaska is no exception. Even though people recently released from prison are some of the most vulnerable to die of a drug overdose, addiction experts say many prisons across the country don’t offer drug treatment.
Organizations like the Ninilchik Community Clinic say they do what they can to care for people entering or leaving jail or prison, but can’t help those inside. And addiction medicine specialists say any interruption in treatment could make it harder for patients to stay in recovery and survive their opioid addiction.
“I really wanted to do good”
Spencer’s patient at the clinic that August day was a woman who asked NPR to use only her first initial, H., because she was critical of the Alaska Department of Corrections and feared retaliation from prison staff. She said she expected to be incarcerated for about 6 months.
H. said there were sometimes contraband drugs in prison and she wanted to get vaccinated to have the best chance of staying sober while incarcerated.
“I wanted to cover my bases, because I really, really wanted to do good,” H. said. “I didn’t want to go back.”
Many studies have shown that medications for opioid use disorder make recovery more likely and reduces the risk overdose deaths.
If people can’t get medication while incarcerated, they could relapse in prison due to black market drugsor, if they don’t use opioids internally, they will detoxification and their tolerance will decrease. This makes them more likely to overdose when they leave.
“No population is more at risk than people who have been recently incarcerated and a lot of that is because … it only takes two weeks for people to lose their tolerance to opioids,” Spencer said.

Dr. Sarah Spencer, peer support specialist Harold Sargeant and case manager Annette Hubbard moved to Nikiski, Alaska on November 20, 2025.
Ash Adams for NPR
hide caption
toggle caption
Ash Adams for NPR
Research supports the idea that people sent to prison are incredibly vulnerable to drug-related death. Federal data released by the Biden administration showed up to 1 in 4 overdose deaths nationally, in 2021, these were people “recently released from jail or prison.” And one National Institute of Health study found that in the weeks following their release from prison, people were up to 40 times more likely to die from an overdose compared to the general population.
H. said treatment for her opioid use disorder was discontinued when she was incarcerated earlier in 2025. She said the Alaska Department of Corrections denied her medication and she returned to using illicit opioids upon her release.
“It happens very quickly,” H. said. “I didn’t have a phone or anything, but you meet people. You see people. It’s just there’s 1,000 different ways.”
Limitations of treatment
Interviews with health care providers like Dr. Spencer and formerly incarcerated people like H. indicate that many who want medications while incarcerated don’t get them.
The Alaska Department of Corrections, or DOC, declined repeated interview requests for this story but responded to questions by email.
They confirmed that they only gave 30 days of drug treatment to people who were already receiving it before their incarceration. No one receives treatment for more than a month unless they are pregnant. When people are released, the DOC said they give some a list of providers they can go to for treatment.
But Spencer said best practice is to make it much easier for any inmate to start and continue taking medications and provide them with a transition plan – such as having DOC schedule an appointment for them with a health care provider in the community – to help them stay safe after release.
“If a patient doesn’t continue to take their medications or isn’t offered medications, you’re really missing that opportunity to stabilize this potentially life-threatening illness while they’re in the care of the DOC,” she said.

Dr. Sarah Spencer and case manager Annette Hubbard discuss various cases between patients. When they’re not seeing patients in the mobile clinic, both spend their time on the phone and on the computer. – follow up with patients, connect them with resources and answer questions.
Ash Adams for NPR
hide caption
toggle caption
Ash Adams for NPR
The DOC said its goal is to expand access to medications for opioid use disorder and hopes to pilot a more comprehensive program by February 2026.
Spencer said that in the absence of comprehensive treatment, his team does its best to provide care to people before and after incarceration, at least on the Kenai Peninsula.
Her colleague Annette Hubbard is a case manager who regularly checks the court docket for active arrest warrants — and helps those she knows with opioid use disorder get treatment before they appear in court.
“I do this voluntarily, because I know the people I work with and for are always in danger,” Hubbard said.
A contrasting approach in Rhode Island
Spencer said she wishes Alaska’s system was more like Rhode Island’s. In 2016, the state began to offer substance use disorder treatment to anyone eligible for DOC care. In one year, there was a 61% reduction in overdose death rates among recently incarcerated people, and a 12% reduction in overdose deaths statewide.
Dr. Jennifer Clarke developed the program as medical director of the Rhode Island Department of Corrections.
Before she could freely dispense medication for substance use disorders, she says, “it was like practicing medicine with one hand tied behind your back.”
According to Clarke, the results of the new program were palpable: When people didn’t suffer from withdrawals or have cravings, they could better focus on their recovery.
“I repeatedly heard people say to me, ‘That was the first time I was really able to participate in the treatment classes, in the behavioral therapy,’” Clarke said.
But she said it wasn’t always easy. The required program two million dollars in financing to start, the support of the governor at the time, and he had to overcome many logistical obstacles. And she said there was a stigma.
“I was often called a drug dealer,” she said. “So with the medical staff, I would just talk about data. I’m like, ‘We’re scientists… We’re going to follow the science.'”
Across the country, unequal access to care
Other states have been slow to develop similar life-saving drug programs. In a recent study published in JAMA Network Openrepresentative of more than 3,000 U.S. prisons, less than half provided some access to medication for opioid use disorder.
Redonna Chandlera psychologist formerly with the National Institute on Drug Abuse, said medications can be difficult to access for anyone with opioid use disorder, and prisons often don’t have providers with the expertise to administer the medications.
“I think it’s still a patchwork of programs,” Chandler said.
And because drugs like buprenorphine are themselves opioids and help ease withdrawal symptoms, there are black markets for them inside prisons and jails.

Case manager Annette Hubbard holds a box of naloxene injections that she says the clinic receives from Remedy Alliance.
Ash Adams for NPR
hide caption
toggle caption
Ash Adams for NPR
“You’ll hear a lot of concerns about ‘diversion’ and diversion of pills, but there are ways to manage and get around this problem, either through alternative formulations or the way you administer the medication,” Chandler said. This could mean switching from pills to injectable formulationswho are much more difficult to divert.
In the meantime, some patients like H. in Ninilchik may only be able to receive treatment outside of incarceration.
“It would be so huge to be able to also be imprisoned and then gain that strength to be able to help yourself when you go back to the streets,” H. said.
It is unclear when she will begin her new prison sentence, but she said she hopes that when she is released, she will immediately return to treatment. If she does, it could save her life.



