A bleak midwinter in London’s hospital corridors of care

Carl MercerBBC Political Editor in London
 BBC
BBCMatthew Trainer thinks it’s the hardest winter he can remember.
He is the chief executive of Barking Havering and Redbridge University Hospitals Trust – and says the number of people coming through the front doors is at a record high.
East London’s two emergency departments, Queen’s Hospital in Romford and King George Hospital in Ilford, experienced their busiest December ever, with almost 1,000 patients requiring treatment each day.
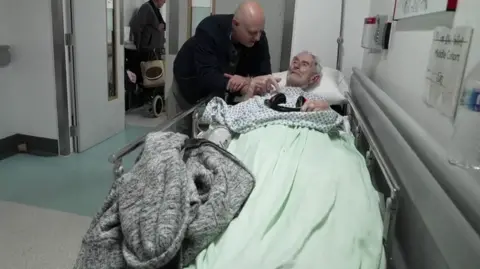
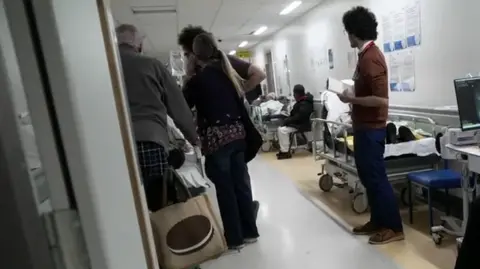
As we walk through Queen’s emergency department, 51 patients are being treated on trolleys in the corridors.
This is the third winter of what we call “hallway care” at the hospital. Corridors have been adapted with new sockets, sinks and emergency alarms to help cope with demand, but Trainer is open about the consequences this brings.
“Corridor care is what causes me the most distress as the hospital CEO and as a human being to parents and family members.
“I hope I never walk on stage walking through these halls and feel upset, because I’ll be worried about my loss of compassion over this. It’s a horrible thing to see.
“It is not acceptable to make someone wait in a corridor overnight on a tram.”
Trainer has asked the government for £35 million to build a new emergency department at Queen’s Hospital.
The Royal College of Nursing said corridor care has become “entrenched” in all English hospitals.

When asked if that description – “grounded” – applies to his confidence, Trainer is cautious.
“It’s difficult because it almost implies that we’re starting to accept it and that’s not the case.
“Our third winter of maintaining the hallways is a horrible place.”
He says staff work around the clock to care for patients in the most dignified and respectful way possible.
“I know that through the messages I receive from patients and their families, they recognize the efforts made by the staff.”
On the day of our visit, we met Cliff Mitchell at 2:00 p.m. GMT, who was there with his elderly father Roy.
Roy had been on a tram in the corridor since 6 p.m. the previous evening.
As his father prepares to leave after treatment, Cliff describes the scene around him.
“There are people everywhere, it seems like organized chaos to me.
“Staff should not work in these conditions, patients should not be treated like this in corridors.
“I couldn’t even stand next to my dad because there was no room…I’m sure everyone struggles with their loved ones.
“People shouldn’t be in the hallways. They should be in a room.”
Ruth Green, director of nursing in the emergency department, echoed that frustration.
“Every year I think it can’t be worse, but it’s been really, really hard.
“Lots of patients, long waits to be seen and lots of waiting times in the emergency room.
“It’s really very, very hard for patients, relatives and staff.”
The pressure is also being felt elsewhere, at Queen’s Hospital.
Around 7,000 babies were born in its maternity ward last year, or around 600 each month.
It is the third busiest unit in the country, with 400 midwives, and received a ‘good’ rating from the Care Quality Commission last December.
The latest arrival arrived just a few hours before our visit.

New parents Holly Chilvers and Sonny Butler are still absorbing the arrival of their eight-hour-old son Landon, who arrived quicker than expected.
“I was like, ‘I’m sorry, I have to get him out,’ and boom, 14 minutes and he was out, first baby,” Holly says.
“Everything went well, perfect,” adds Sonny.
“It was really a shock when it first came out. I had trouble holding it but the lady showed me how to do it.”
Maternity unit manager Kathryn Tompsett said the service was looking at how to provide care in the “most efficient way” amid near-constant NHS budget pressures.
Effectiveness, she adds, is also “often the best care for women and their families.”

At the trust’s sister hospital in Ilford, another approach to easing pressure is underway.
King George Hospital is home to the Elective Surgery Centre, a nine operating theater unit dedicated only to planned operations. By separating them from emergency works, the trust hopes they are less likely to be disrupted.
More than 10,000 planned operations were carried out at the hub last year, helping to reduce waiting lists.
Former nurse Stuart Ayris was preparing to have a knee replacement when we met him. He said he was impressed by how quickly his operation was organized.
“I’ve been playing cricket for 12 years. I have a terrible batting average, so I hope it improves,” he tells us.
The operation was led by orthopedic consultant Sivakumar Shankar, assisted by a robot, one of the few in the capital.
“This helps us decide which implant should be the right one, based on detailed imaging of the patient,” he explains.

“I tell the robot what to do, and then it does it. This helps us make the operation even more precise.”
As the team drilled and shaped the bone to fit the replacement, the technology offered a glimpse of progress in a live system.
Some challenges at Queen’s and King George are being resolved.
Others, including the long-standing reliance on corridor maintenance, remain a work in progress.
Although Trainer’s £35m bid for a new emergency department could ease the pressure at Queen’s Hospital, he says the deeper challenge lies elsewhere: finding ways to stop so many people having to go to hospital in the first place.




