‘A second set of eyes’: AI-supported breast cancer screening spots more cancers earlier, landmark trial finds

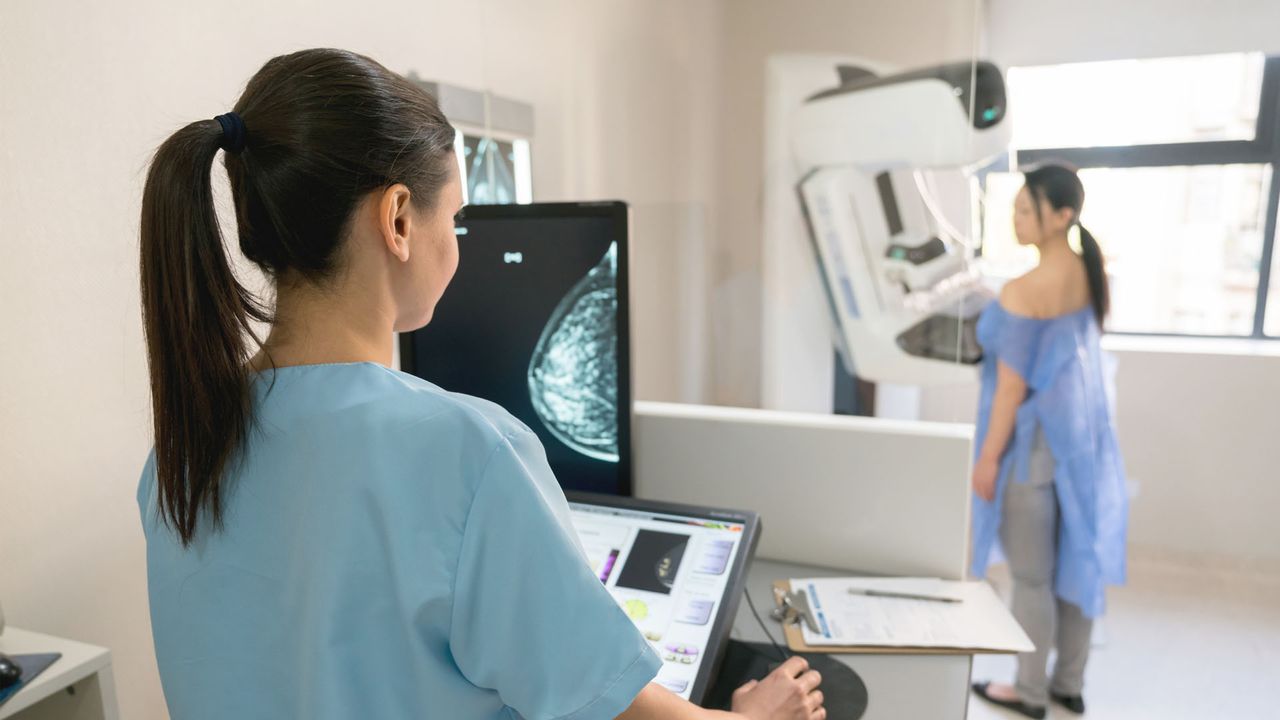
First-of-its-kind trial demonstrates that AI-assisted mammography can improve outcomes for breast cancer patients, particularly those with aggressive disease.
Although many people have only recently started using artificial intelligence (AI) in their daily lives, the use of this technology in medicine began around ten years ago, particularly in the field of image-based diagnosis. Researchers have trained AI programs to recognize tumors and other signs of disease in various medical images, such as X-rays, MRI scans, and tissue biopsies mounted on slides.
However, knowing whether an AI tool can actually diagnose cancer and make a difference for patients requires a “prospective” study – one in which patients diagnosed using the AI tool are then followed for several years to determine their health outcomes.
Now, Swedish researchers have conducted a landmark trial to evaluate the use of AI in mammography screening. Results of the Mammography Screening with Artificial Intelligence (MASAI) trial, published January 31 in the journal The Lancetshowed that AI-assisted mammogram reading can improve screening performance while reducing radiologists’ workload.
This is the first time AI has been shown to improve outcomes for breast cancer patients.
Detect cancer earlier
The practice of regularly screening patients has significantly reduces the incidence of advanced cancers and deaths from breast cancer in much of the world. But even with regular mammograms, some cancers can go unnoticed.
These “interval cancers” are not detected during an initial screening but are diagnosed in the following two years, or between two screening cycles. They are often missed because they are hidden during the initial screening due to the density of the breast tissue or the tumor disguising itself as normal tissue. Or sometimes, they can grow very quickly between screening dates.
These cancers are invasive, spread to nearby healthy tissues, and are generally aggressive, leading to worse patient outcomes. Declining interval cancer rates is the best way to confirm that a screening method is working, meaning it reduces late-stage cancer diagnoses by detecting more cases earlier.
“If you want to improve the effectiveness of screening, the interval cancer rate is a very good surrogate measure of breast cancer mortality,” said the study’s lead author. Dr. Kristina Langbreast radiologist and clinical researcher at Lund University in Sweden, told Live Science. “So if we can reduce interval cancers, that will likely have a positive impact on patient outcomes.”
The MASAI trial included more than 100,000 women aged 40 to 80 living in Sweden. It used a commercially available AI system that was trained on more than 200,000 exams performed at medical facilities around the world.
In a control group, mammograms were read by two radiologists, as is standard in Sweden. In the AI-assisted group, the AI system analyzed mammograms for suspicious findings and provided a risk score of 1 to 10. Cases with a score of 1 to 9 were then read by a single radiologist, while a score of 10 was read by two radiologists. The AI system was also able to highlight suspicious findings in the image so that human radiologists could examine them easily.
AI-supported screening identified more clinically relevant cancers than unassisted mammography. “Clinically relevant” cancers are those that have the potential to progress and therefore require medical intervention.
This also reduced the number of interval cancer diagnoses within two years of screening. This shows that the AI program was more effective in identifying cancers that might normally be missed by a human radiologist, allowing medical treatments to begin sooner.
Reduce false positives
Although cancer screening is generally beneficial, it has some potential disadvantages, such as false positives and overdiagnosis. When a patient is called back for another check-up after a screening but doesn’t have cancer, “it can be a really stressful experience,” Lång said.
This last situation, overdiagnosis, refers to situations where a screening detects a cancer that will ultimately not cause any harm to the patient. Such cancers grow so slowly that they will not cause symptoms during the patient’s lifetime and will not increase the risk of death. Overdiagnosis can subject healthy patients to unnecessary cancer treatments.
The goal of AI-assisted mammography is to improve the screening test’s ability to detect cancer while mitigating these potential negative effects – and the study found that AI-assisted screening did not increase the risk of false positives and that it improved detection of clinically relevant cancers.
In addition to improving cancer detection, AI-assisted screenings could address ongoing problems shortage of radiologists available for cancer screening.
“In some places, you’re lucky to find a radiologist to read mammograms,” said Dr. Richard Wahla radiation oncologist from Washington University in St. Louis who was not involved in the study. “If you don’t have expert radiologists, women can’t benefit from screening programs as they should.”
Additionally, as the few available radiologists work more hours, their performance decreases. But the AI does not get tired and its performance does not decline at the end of the working day.
“The labor problem is real, and that [study] This could have an impact,” Wahl said. “I think people will gradually be interested in AI-assisted interpretation as a second pair of eyes.”
Lång and his team will begin a screening trial in Ethiopia in March, where they will use AI to support the rapid assessment of breast cancer using bedside ultrasound scans as part of a screening program.
“The problem in these settings where there is no screening program is that many women arrive with advanced disease and there are no radiologists on site,” Lång said. With the support of AI, Lång hopes to improve access to accurate screening and thus enable earlier diagnosis of breast cancer in these resource-limited settings.
This article is for informational purposes only and is not intended to offer medical advice.
Gommers, J. et al. (2026). Interval cancer, sensitivity and specificity comparing AI-assisted mammography screening with standard double reading without AI in the Masai study: a randomized, controlled, non-inferiority, single-blind, population-based screening accuracy trial. The Lancet, 407(10527), 505-514. https://doi.org/10.1016/s0140-6736(25)02464-x




