Colon cancer is killing more young people in the U.S. than any other cancer

Most types of cancer have become less deadly over time among adults under 50 in the United States, but colon and rectal cancers continue to claim lives at an alarming rate, according to a new report from the American Cancer Society. Data shows that colorectal cancer has officially become the leading cause of cancer deaths among young people.
The report analyzes annual U.S. death rates from 1990 to 2023 for the five deadliest cancers in men and women under 50 — an age group that researchers have tracked to understand early-onset cancer risk. Encouragingly, cancer mortality in this age group as a whole has decreased by 44 percent. But rates of colorectal cancer among young people have risen steadily in recent decades, and the disease has gone from the fifth leading cause of cancer deaths in 1990 to the leading cause in 2023.
“This is an inflection point,” says William Dahut, scientific director of the American Cancer Society. “This is the first time it has been the number one cancer death in people under 50.”
On supporting science journalism
If you enjoy this article, please consider supporting our award-winning journalism by subscription. By purchasing a subscription, you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
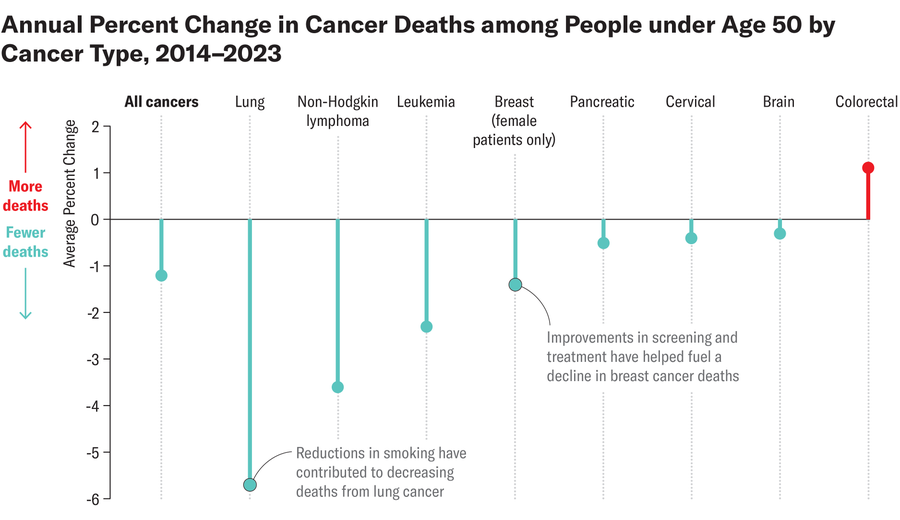
Amanda Montañez; Source: “Leading Cancer Deaths Among People Under Age 50,” by Rebecca L. Siegel et al., in JAMA. Published online January 22, 2026 (data)
Deaths from all other major cancers, including breast, lung and pancreatic cancers, have declined, which Dahut attributes largely to improvements in therapies. “I think this is another important statement that our investment as a nation in science to develop better treatments is paying off in our young adults,” he says.
Contrary to these positive trends, the colorectal cancer mortality rate is the only one to have worsened. The results show that it is the leading cause of cancer death in men and the second leading cause of cancer death in women after breast cancer – and has become the leading cause of cancer death in the general population. Many of the cancers studied, including colorectal cancer, are typically seen later in life, between ages 60 and 70, says Jeff Meyerhardt, a gastrointestinal oncologist and co-director of the Colon and Rectal Cancer Center at Dana-Farber Cancer Institute.
“They are considered cancers of aging,” he says. “At least in the case of colorectal cancer, age [of onset] has been fixed for a while, until more recently.
Since the 1990s, cases of colorectal cancer in people under 50 have increased steadily by about 2% per year. And the majority of cases are diagnosed at later stages, when they are more difficult to treat.
“About three-quarters, maybe 60 to 70 percent of the time, people [under age 50] “Unfortunately, this is what I expected,” says Andrea Cercek, founder and co-director of the Center for Early-Onset Colorectal and Gastrointestinal Cancer at Memorial Sloan Kettering Cancer Center. Despite advances in the treatment of colorectal cancer, the survival rate in advanced stages of the disease is still low.
Delayed diagnosis is likely a factor in more severe and fatal cases. In the United States, it is recommended to begin screening for colorectal cancer, usually with a colonoscopy, at age 45 for most people without a genetic or family history of the disease. This recommended age was lowered by 50 years just a few years ago in response to increasing incidence rates in younger age groups. Younger people with colorectal cancer may not seek medical attention if they experience symptoms such as bleeding in the stool, difficult bowel movements, bloating, or signs of anemia, all of which can sometimes be confused with other health problems. And doctors might not consider screening these people for colorectal cancer because their age puts them at lower risk, Meyerhardt says.
But some researchers think there’s more to it than late diagnosis.
It usually takes years for a colorectal polyp, or small growth, to turn into a cancerous tumor, Dahut explains. Scientists are trying to understand when exactly tumor growth begins and how quickly it spreads if cancer occurs at a much younger age than in the past. Cercek says data shows the biggest increase in cases has occurred among 20- to 30-year-olds.
“If you think about the typical process, say, for a 22-year-old person, the polyp should have shown up literally at age 10,” she says. It’s plausible but difficult to detect without screening people at a very young age, but there could also be a difference in the progression of the tumors themselves, Cercek says. “We are very interested to see if there is anything in the process that could be more accelerated, that could be different,” she adds.
Scientists are investigating several possible explanations for this trend, including diet, exercise, lifestyle, genetics, environmental factors, and even microplastics and antibiotics. But many researchers agree that there is no single cause. We hope that focusing on credible factors will lead to more targeted screening of younger people at high risk for the disease, without increasing false positives or unnecessary surgeries or colonoscopies, says Meyerhardt.
Cercek adds that improving therapies so that they are less toxic to patients, as well as providing emotional and social support during recovery, will be crucial as the number of young people facing colorectal cancer continues to rise.
“What’s happening as a whole is alarming. But it’s extremely important to recognize that surviving as a young adult with colorectal cancer is life-changing. It’s incredibly difficult and can be incredibly taxing emotionally, physically and financially,” she says. “The earlier we can diagnose, the better it will be for our patients. »
And perhaps such improvements in treatment and detection will eventually bring colorectal cancer survival in line with that of other cancers.



