Medicaid Work Rules Exempt the ‘Medically Frail.’ Deciding Who Qualifies Is Tricky.

Eliza Brader fears she will soon have to prove she is working to continue receiving Medicaid health coverage. She doesn’t think she should have to.
The 27-year-old Bloomington, Indiana, resident suffers from a pacemaker and a painful joint condition. She also fused vertebrae in her neck following a spinal injury, preventing her from turning her head.
Indiana’s Medicaid agency currently considers Brader “medically fragile,” giving him access to an expanded set of benefits, such as physical therapy.
The new federal rules will require more than 18 million Medicaid enrollees nationwide to show they work, volunteer or go to school 80 hours a month starting in 2027 to maintain coverage. Brader is exempt as long as she is deemed medically fragile.
But lacking sufficient federal guidance, states are grappling with how to define medical frailty — a consequential decision that could reduce Medicaid coverage for many people, state officials, consumer advocates and health policy researchers said.
“It’s terrifying,” Brader said. “I already fought very hard to get my health care. »
“Incredibly high” stakes
President Donald Trump’s One Big Beautiful Bill Act cuts nearly $1 trillion from Medicaid over the next decade, with much of the savings expected to come from not covering those who don’t qualify under the new work rules. These spending cuts help offset the costs of Republican Party priorities, such as overseas security and tax cuts that primarily benefit the wealthy.
Conservative lawmakers have argued that Medicaid, the government health insurance program for low-income or disabled people, has become too large and too expensive, particularly following its expansion to more low-income adults under the Affordable Care Act. They also say that requiring participants to work is common sense.
Work rules contained in the Trump tax and spending law provide exemptions to several groups who might have difficulty complying with them, including people considered “medically fragile.” The law spells out certain “medically fragile” conditions such as blindness, disability, and substance use disorders. But he doesn’t list many others.
Instead, the law exempts people with a “serious or complex health condition,” a term whose interpretation can vary by state.
State officials say they need more clarity to ensure people who can’t work for health reasons maintain legitimate access to Medicaid. They also fear that, even with a clear definition, people will face the burden of regularly having to vouch for their fragile health, which is a challenge without reliable access to medical care.
“The stakes are incredibly high,” said Kinda Serafi, a partner at consulting firm Manatt Health.
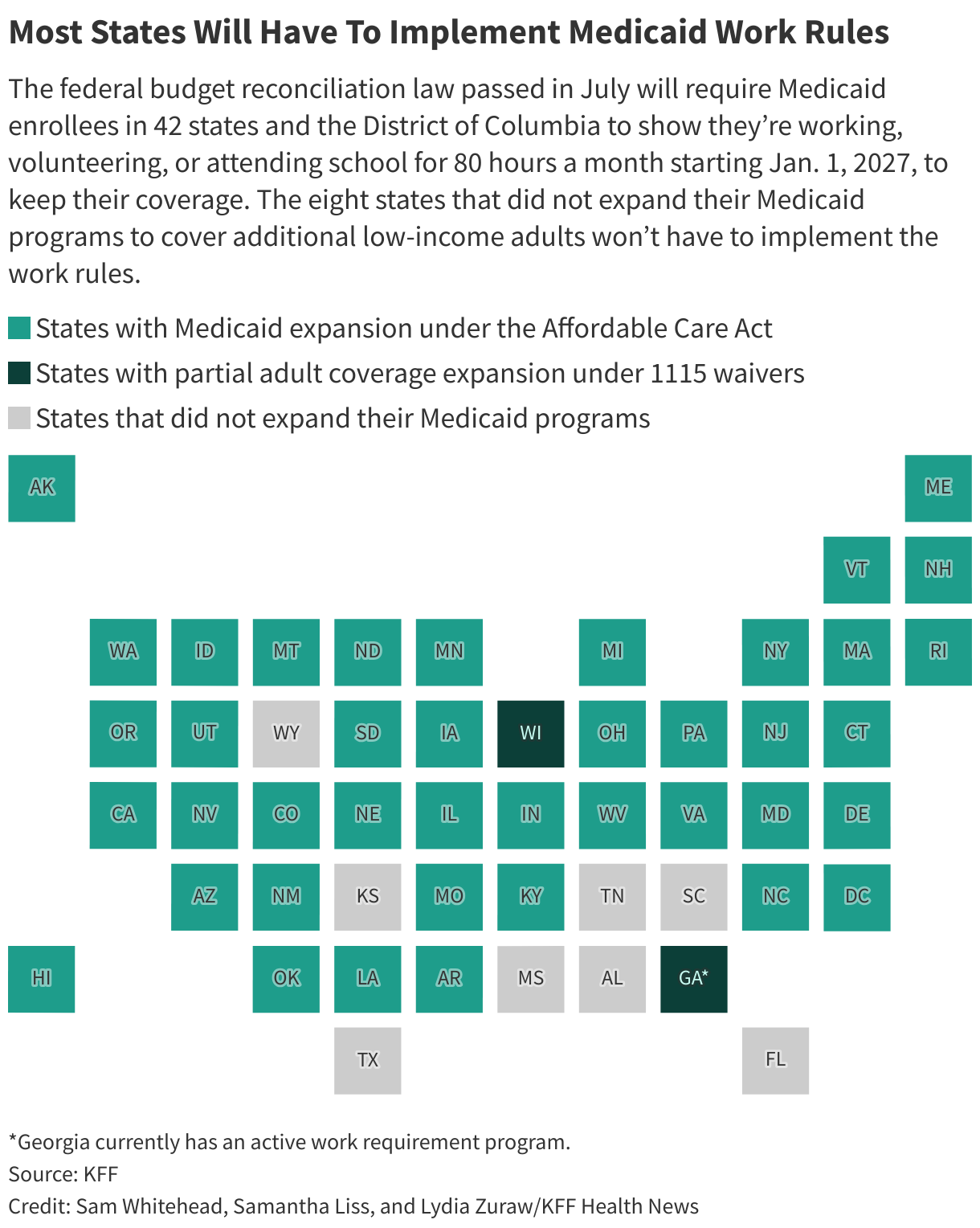
The new work requirements will affect Medicaid beneficiaries in 42 states and Washington, D.C. Eight states – Alabama, Florida, Kansas, Mississippi, South Carolina, Tennessee, Texas and Wyoming – have not expanded their Medicaid programs to cover more low-income adults, so they will not have to implement the work rules.
Medicaid work rules are expected to be the main driver of health insurance coverage losses over the next decade, according to the nonpartisan Congressional Budget Office.
According to KFF, forty-four percent of all adults covered by state expanded Medicaid programs have at least one chronic health condition.
A challenge for States
State Medicaid agencies are scrambling to implement the rules with little guidance from the U.S. Department of Health and Human Services, which has yet to issue specific guidance. Federal officials will clarify the definition of “medically fragile” next year, said Andrew Nixon, an agency spokesman.
Ultimately, states will have to decide who is unhealthy enough to be exempt from work rules. And it won’t be easy for officials and their computer systems to follow.
Each year, state eligibility systems review millions of applicants to see if they qualify for Medicaid and other government programs. Now, these same systems must screen existing applicants and registrants to determine whether they meet the new work rules.
Jessica Kahn, a partner at consulting firm McKinsey & Co., urged states to start planning how to adapt eligibility systems to verify work status. States can do a “tremendous amount” of work without direction from the federal government, said Kahn, a former federal Medicaid official who spoke at a recent Medicaid advisory committee hearing. “Time is already a waste.”
State Medicaid directors are considering the challenge.
“Medical frailty is becoming so complex,” Emma Sandoe, Oregon’s Medicaid director, said during a recent panel discussion. Conditions that can prevent people from working, such as mental health disorders, can be difficult to prove, she said.
A state could try to use data extracted from a person’s health records, for example, to determine their medical frailty. But the information in a patient’s record may not provide a clear picture of a person’s health, especially if they don’t have regular access to medical care.
That’s a tall order for eligibility systems that historically haven’t needed to dig through medical records to screen applicants, Manatt Health’s Serafi said.
“It’s an incredibly new thing that registration systems just don’t get a handle on at all,” Serafi said.
Lobbying groups for private health insurance companies that help manage Medicaid in many states have also urged federal regulators to clearly define medical frailty so it can be applied uniformly.
In a Nov. 3 letter to federal officials, Medicaid Health Plans of America and the Association for Community Affiliated Plans argued for allowing enrollees to qualify for the waiver by indicating on their applications that they have conditions that make them medically fragile. Successfully implementing exemptions for the medically fragile will be “crucial” given the “serious health risks of loss of coverage for these populations,” the groups said.
Some state officials worry about unintended consequences of work rules for people with chronic illnesses.

Jennifer Strohecker, who recently resigned as Utah’s Medicaid director, reiterated the high stakes, especially for people with diabetes on Medicaid. They may be very healthy and functional on insulin, but if they fail to meet work requirements, that may change, Strohecker said at a recent Medicaid advisory hearing.
Whether someone is considered medically fragile already depends largely on where they live.
For example, in Arkansas, people indicate on their Medicaid applications that they are disabled, blind, or need help with daily activities.
About 6 percent of the approximately 221,000 people enrolled in Arkansas’ Medicaid expansion program are considered medically fragile, according to Gavin Lesnick, a spokesman for the Arkansas Department of Human Services.
In West Virginia, the state accepts a medical fragility designation when an applicant self-declares it.
The burden of proof is higher in North Dakota. Applicants must complete a health questionnaire and submit additional documentation, which may include medical record notes and treatment plans. More than half of applicants were turned away last year, according to Department of Health and Human Services spokeswoman Mindy Michaels.
Indiana’s Family and Social Services Administration, which runs its Medicaid program, declined an interview and said it cannot comment on individual cases, like Brader’s.
Brader fears the additional paperwork could cause him to lose Medicaid again. She said she was temporarily kicked out of the program in 2019 for failing to follow state work rules when Indiana said her work-study job didn’t count as employment.
“Every time I’ve tried to get help from the state of Indiana, it’s been a bureaucratic nightmare,” she said.
As states await federal guidance, Kristi Putnam, a senior fellow at the conservative Cicero Institute and former secretary of the Arkansas Department of Human Services, which oversees the state’s Medicaid program, said that even if a state creates a long list of medically fragile conditions, the line must be drawn somewhere.
“You can’t create a policy of exemptions that applies to everything,” she said.