Rural Health Providers Could Be Collateral Damage From $100K Trump Visa Fee

Bekki Holzkamm has been trying to hire a lab technician at a hospital in rural North Dakota since the end of the summer.
No U.S. citizens applied.
West River Health Services in Hettinger, a town of about 1,000 in the southwest part of the state, has four options, and none of them are good.
The hospital could pay more than $100,000 for the new H-1B visa fees imposed by the Trump administration and hire one of more than 30 applicants from the Philippines or Nigeria. The fee is the equivalent of what some rural hospitals would pay two lab technicians a year, said Holzkamm, West River lab director.
West River could ask the Department of Homeland Security to waive the fee. But it is unclear how long the waiver process would take and whether the government would grant it. The hospital may continue to try to recruit someone in the United States for the position. Or, Holzkamm said, it could leave the position vacant, increasing the workload on the current “skeleton team.”
The U.S. health care system depends on foreign-born professionals to fill its ranks of doctors, nurses, technicians and other health care providers, especially in chronically understaffed facilities in rural America.
But a new presidential proclamation targeting the tech industry’s use of H-1B visas makes it harder for West River and other rural providers to hire that staff.
“The health care industry hasn’t even been considered. It’s going to be collateral damage, and to such an extreme degree that it clearly hasn’t been thought about at all,” said Eram Alam, an associate professor at Harvard whose new book examines the history of foreign doctors in the United States.
Elissa Taub, a Memphis, Tenn.-based attorney who helps hospitals with the H-1B application process, has heard her clients’ concerns.
“It’s not like there’s a surplus of American doctors or nurses waiting in the wings to fill these positions,” she said.
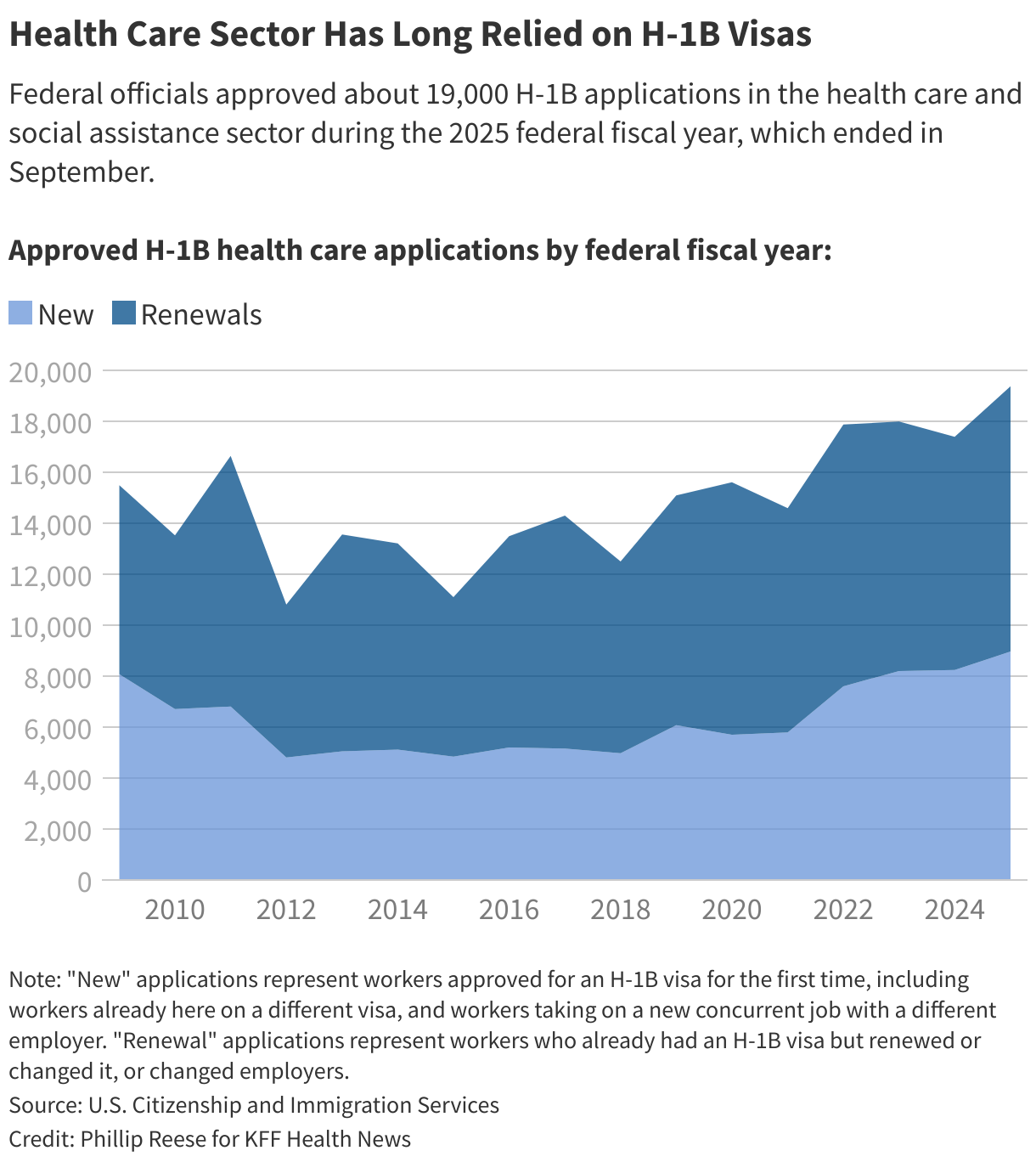
Until recently, West River and other employers paid up to $5,000 each time they applied to sponsor an H-1B worker. Visas are reserved for highly skilled foreign workers.
The new $100,000 fee — part of a proclamation from President Donald Trump in September — applies to workers living outside the United States, but not to those who were already in the United States on a visa.
Kathrine Abelita, a lab technician from West River, is one of nine hospital employees – six technicians and three nurses – who are current or former H-1B visa holders. Abelita is originally from the Philippines and has worked at West River since 2018. She is now a permanent resident of the United States.
“This is going to be a big problem for rural health care,” she said of the new fees. She said most young American workers want to live in urban areas.
Sixteen percent of registered nurses, 14% of physician assistants and 14% of nurse practitioners and midwives who work in U.S. hospitals are immigrants, according to a 2023 government survey. In the United States, nearly a quarter of doctors studied medicine outside the United States or Canada, according to 2024 licensing data.
The American Hospital Association, two national rural health organizations and more than 50 medical societies have called on the administration to grant the health care industry exemptions from the new fees. The new cost will disproportionately harm rural communities that already struggle to afford and recruit enough providers, the groups say.
“A general exception for health care providers is the easiest route,” the National Rural Health Association and the National Association of Rural Health Clinics wrote in a joint letter.
The proclamation allows fee waivers for individuals, workers of specific companies, and those of entire sectors when “in the national interest.” New guidance says fees will only be waived in “extraordinarily rare circumstances.” That includes showing that there are “no American workers” available for the job and that requiring a company to spend $100,000 would “significantly harm” U.S. interests.
Taub called those standards “exceptionally high.”
Representatives of the NRHA and the American Medical Association, who organized a letter from the medical societies, said they received no response after sending requests to Homeland Security Secretary Kristi Noem in late September and early October. The AHA declined to say whether it had received a response.
Homeland Security officials referred KFF Health News’ inquiries to the White House, which did not respond to questions about individual waiver deadlines or the possibility of a categorical exemption for the health care sector.
Instead, White House spokesperson Taylor Rogers sent a statement defending the new fees, saying they would “put American workers first.” His comments echo Trump’s proclamation, which focuses on accusations that the tech industry is abusing the H-1B program by replacing American workers with lower-paid foreigners. But the order applies to all professions.
Alam, the Harvard professor, said the United States’ reliance on international providers raises legitimate concerns, including how it drives professionals away from lower-income countries, which face even more severe health problems and staffing shortages than in the United States.
This decades-long dependence, she explained, stems from the population boom, the historic exclusion of nonwhite men from medical schools, and the “much, much cheaper” cost of importing foreign-trained providers than of expanding health education in the United States.
Foreign-trained doctors tend to work in poor, underserved rural and urban areas, according to a survey and research review.
Nearly 1,000 H-1B providers were employed in rural areas this year, the two rural health organizations wrote in their letter to the Trump administration.
J-1 visas, the most common type held by foreign doctors during residencies and other postgraduate training in the United States, require them to return to their home country for two years before applying for an H-1B visa.
But a government program called the Conrad 30 Waiver Program allows up to 1,500 J-1 holders per year to stay in the United States and apply for an H-1B in exchange for three years of work in a provider shortage area, which includes many rural communities.
Trump’s proclamation indicates that employers who sponsor H-1B workers already in the United States, such as doctors receiving these waivers, will not have to pay the six-figure fee, a nuance clarified in guidance issued about a month later.
But employers will have to pay the new fees when hiring doctors and others applying while living outside the United States.
Alyson Kornele, CEO of West River Health Services, said most of the foreign nurses and lab technicians she hires are outside the United States when they apply.
Ivan Mitchell, CEO of Great Plains Health in North Platte, Nebraska, said most of his hospital’s H-1B doctors were in the United States on other visas when they applied. But he said physiotherapists, nurses and lab technicians usually apply from abroad.
Holzkamm said it took five to eight months to hire H-1B applicants at his lab before the new fees were introduced.

Bobby Mukkamala, a surgeon and president of the American Medical Association, said Republican and Democratic lawmakers were concerned about the implications for rural health care.
Among them, Senate Majority Leader John Thune said he plans to discuss possible exemptions.
“We want to make it easier, not harder, and less expensive, not more expensive, for people who need labor,” the Republican told KFF Health News in September.
Thune’s office did not respond to questions about whether the senator had heard from the administration regarding possible waivers for health care workers.
The Trump administration faces at least two lawsuits trying to block the new fees. One group of plaintiffs includes a company that recruits foreign nurses and a union that represents medical graduates. Another lawsuit, filed by the U.S. Chamber of Commerce, cites concerns about doctor shortages and the ability of health systems to pay the new fees.
Kornele said West River would not be able to pay a $100,000 fee so it would double down on local recruitment and retention.
But Holzkamm said she hasn’t been able to find lab technicians at North Dakota colleges, even those who intern at the hospital. She said West River couldn’t compete with the salaries offered in big cities.
“It’s a bad cycle right now. We have a lot of problems,” she said.
Phillip Reese is a data reporting specialist and associate professor of journalism at California State University-Sacramento.