Goats and Soda : NPR
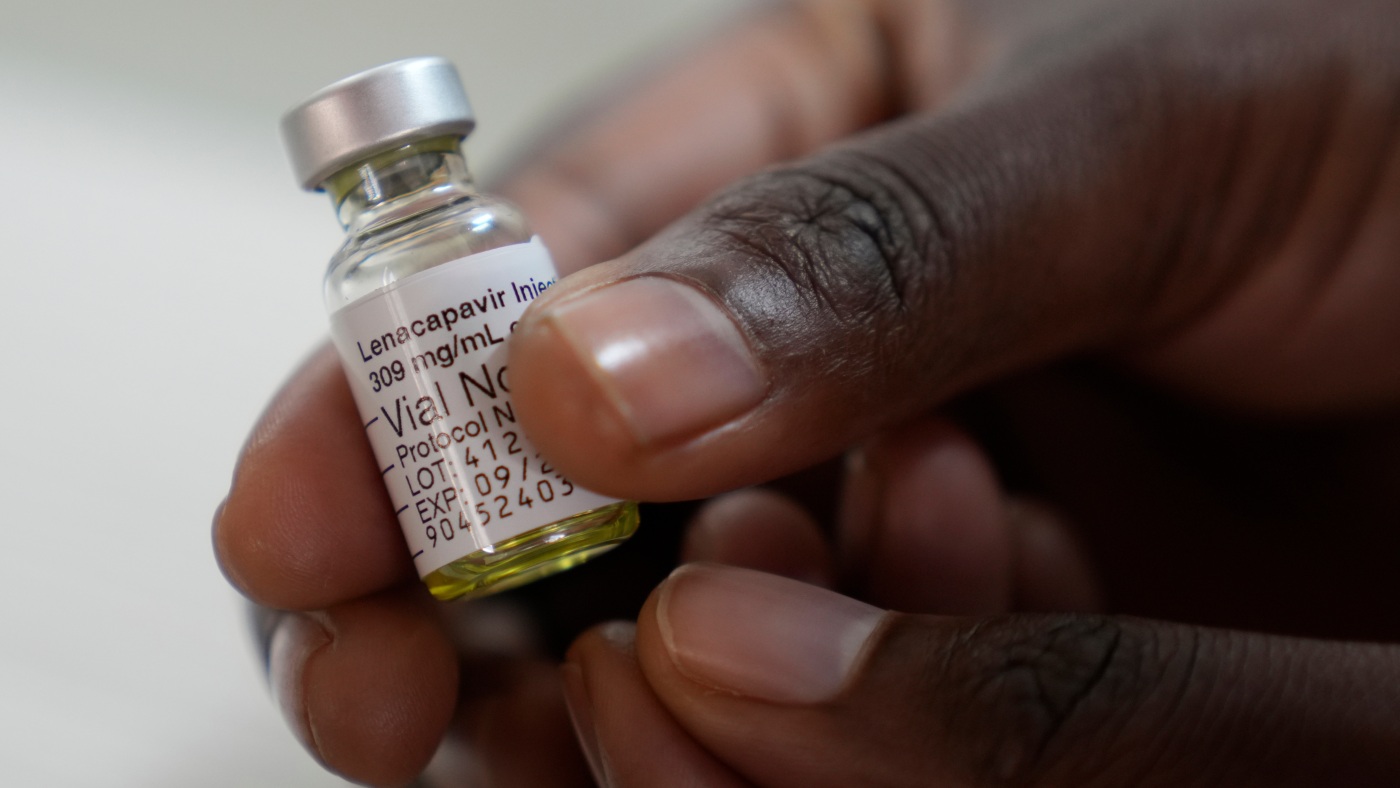

A pharmacist holds a vial of lenacapavir, described as a “revolutionary” HIV prevention drug, at a research site in South Africa.
Nardus Engelbrecht/AP
hide caption
toggle caption
Nardus Engelbrecht/AP
Five months after a “breakthrough” HIV prevention drug was approved in the United States and became available in many wealthy countries, it is being rolled out in two African countries particularly hard hit by the disease.
On Wednesday, the US State Department announced that Eswatini and Zambia had each received 500 doses of lenacapavir, a drug made by Gilead Sciences that has been hailed as Science like a “breakthrough“Just two injections per year provide almost complete protection against HIV infection.
“It’s somewhat unprecedented to see a global health innovation spread so quickly to low- and middle-income countries,” says Mitchell Warren, executive director of the AIDS Vaccine Advocacy Coalition (AVAC), a global HIV prevention organization. “Obviously very small amounts, really just a down payment, but these are the first of what we believe will be many doses in these two countries and other countries.”
The delivered doses mark the first small step toward providing at least 2 million doses to the most affected countries, primarily in Africa, by 2028. This is the goal of the Global Fund, a major donor in the fight against HIV, tuberculosis and malaria, alongside Gilead Sciences and the State Department.
But this breakthrough drug comes “at a time when we have witnessed some of the most dramatic political and economic challenges in the AIDS response,” Warren says. In addition to likely increasing the overall HIV burden due to care disruption, Warren says the Trump administration’s foreign aid cuts have damaged some of the systems and programs best positioned to get lenacapavir to people who need protection most. “We’re starting from a deficit that we didn’t need, that was entirely the fault of the U.S. government.”
Fast delivery
The State Department announced its investment in lenacapavir in September, committing to supply up to 2 million doses by 2028.
“We believe we will achieve this goal in mid to early 2027. [and] we’re going to collectively purchase over half a million doses next year,” Jeremy Lewin, a senior official for foreign aid, humanitarian affairs and religious freedom at the State Department, said at a press briefing this week.
The 500 doses are being provided by Gilead at cost, with no profit to the company, according to CEO Daniel O’Day. The company plans to cover up to 2 million doses in total before approved generics are up and running, but it’s unclear how many doses they currently have on hand. “We have supplies to send to markets when they have the appropriate regulatory approval, as well as a resupply for Eswatini and Zambia,” he said at the press briefing.
Since the FDA administered lenacapavir thumbs up in June (followed by World Health Organization And European Medicines Agency in July), Gilead has filed for regulatory approvals across sub-Saharan Africa. So far, Zambia and South Africa have approved the drug (Lewin said the United States was not considering funding doses of lenacapavir in South Africa, which would be encouraged “to fund doses for their own population.”) The Eswatini Department of Health issued a separate import authorization, their version of approval.
Where will the medicine go next? The company has applied for approval in Botswana, Kenya, Malawi, Namibia, Rwanda, Tanzania, Uganda and Zimbabwe, with more in the works, O’Day said. “We continue to prioritize 18 high-burden countries, which account for 70% of the HIV epidemic.”
Of course, delivery is only the first step. To curb the epidemic, doses must reach the people who need them.
The ministries of health will be primarily responsible for this. But in many cases, governments have relied on help from community agencies and non-governmental organizations. The State Department’s Lewin said it was part of the America First global health strategy’s efforts to strengthen the “autonomy” of the national government.
Yet many health systems rely on outside organizations that have been starved of funding or diminished by the Trump administration’s foreign aid cuts, Warren says. That includes one that his organization, AVAC, helped implement. The program aimed to strengthen the capacity of health systems to provide injectable HIV drugs, such as lenacapavir, which can be more difficult to distribute than pills. It was frozen out in January, he said, and has not returned to full capacity.
“If you don’t have a program that meets people where they are, then those doses aren’t going to be used,” Warren says. “There’s a long history of global health products that everyone finds exciting, and then they sit in stores because we haven’t built the program to deliver them.”


